## **What is EM Coding?**
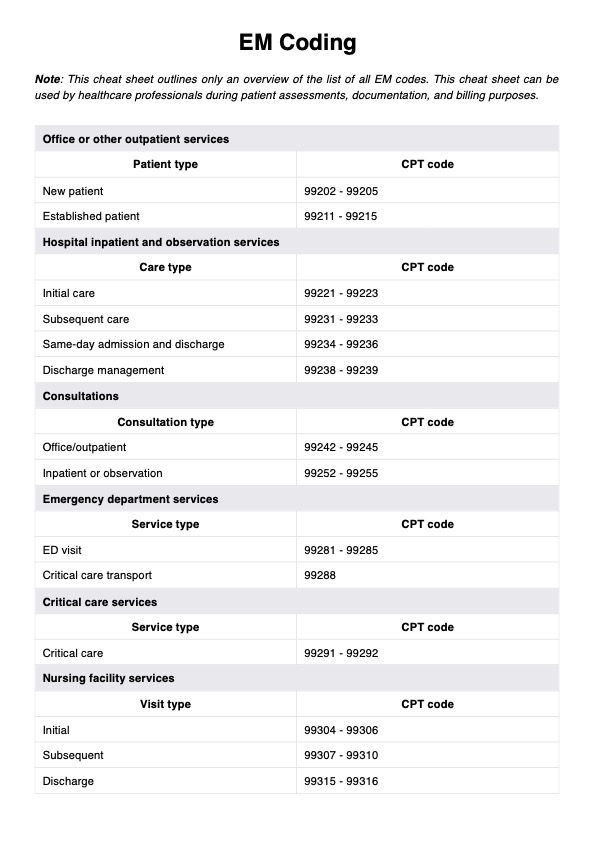
Evaluation and Management (E/M) coding is a system used by medical professionals to document and bill for non-procedural services related to assessing and managing a patient’s health. These evaluation and management services are assigned CPT codes ranging from 99202 to 99499 and cover a variety of encounters, including office visits, hospital inpatient services, home visits, and preventive care.
Unlike codes used for surgeries or diagnostic tests, E/M codes also reflect cognitive work—such as history-taking, examinations, and medical decision-making—that healthcare professionals perform during patient consultations. E/M coding plays a critical role in medical billing because it directly influences the reimbursement clinicians receive from Medicare, Medicaid services, and private insurers.
Accurate use of these services provided helps ensure fair payment and protects against issues like underbilling, overbilling, or audit triggers. The E/M coding system has evolved since its original documentation guidelines were introduced in 1995, with notable updates in 1997, 2021, and 2023 aimed at simplifying documenting clinical information and aligning it more closely with actual clinical work (American Academy of Professional Coders, 2024).
Health care providers select E/M codes based on factors such as whether the patient is new or an established patient, the outpatient setting, and either the complexity of medical decision making or total time spent. Proper management, coding, and documentation support the chosen code and ensure billing compliance.
## **EM Coding guidelines**
Evaluation and management (E/M) coding guidelines provide a structured approach to documenting and billing non-procedural management services. These codes apply to encounters where a provider evaluates and manages patient health, including office visits, hospital observation services, home visits, and preventive services. The correct E/M code is selected based on several key factors: patient type (new vs. established patient), the care setting (e.g., outpatient services, hospital, emergency department), and either the complexity of medical decision making (MDM) or the total time spent by the provider on the date of the patient encounter.
Medical decision-making is a core determinant of the E/M code level. It considers the number and complexity of problems addressed, the volume and complexity of data reviewed, and the potential risks associated with managing patient health. Alternatively, total provider time—including both face-to-face and qualifying non-face-to-face activities—can be used to determine the code selection when appropriate. Documentation should clearly reflect the patient's history, physical exam findings, the medical decision-making process, and any counseling or care coordination provided.
Guideline updates in 2021 and 2023 simplified E/M coding by revising documentation guidelines and eliminating redundant hospital observation services codes. Providers should also be aware of newer additions, like add-on code G2211 (effective 2024), used for complex other outpatient evaluation services. Accurate documentation and medical necessity remain essential to ensure compliance and proper reimbursement.
## **How does it work?**
Carepatron’s E/M Coding Cheat Sheet is designed to streamline clinical documentation and medical billing by giving practicing health care providers instant access to up-to-date CPT codes for evaluation and management services. With just a few steps, you can integrate this tool into your daily workflow to ensure accurate, compliant E/M coding.
### **Step 1: Access the cheat sheet**
Click the “Use template” button on this page to instantly open the E/M Coding Cheat Sheet in Carepatron where you can customize it to add more codes or make other edits. You can also click "Download" to instantly get a PDF copy.
### **Step 2: Use the cheat sheet in patient assessment**
During patient encounters, use the cheat sheet to quickly determine the appropriate E/M code based on setting, patient type, medical decision making, or time spent. Whether documenting emergency department visits, hospital inpatient services, or nursing facility services, the cheat sheet ensures fast, compliant code selection during direct patient contact.
### **Step 3: Discuss the content of the cheat sheet**
If your team or practice shares documentation guidelines, reviewing the cheat sheet together promotes consistency across all health care providers. It’s ideal for onboarding, team huddles, or staying aligned with updates from the American Medical Association and CMS on evaluation and management services.
### **Step 4: Provide patient support if needed**
Accurate E/M coding minimizes claim denials and delays, enhancing the patient experience. If patients have concerns about charges or coverage, medical service providers can reference documented services provided, including independent interpretation, separately obtained history, and primary service time, supporting transparent communication.
## **Who uses EM Coding?**
EM Coding is used by various stakeholders within the healthcare industry, including:
- **Healthcare providers**: Physicians, nurse practitioners, physician assistants, and other qualified healthcare professionals use E/M coding to document and bill for the evaluation and management services provided during patient encounters. They must accurately assign E/M codes based on the complexity of the visit and the level of medical decision making involved.
- **Medical coders and billers**: They play a crucial role in medical billing, reviewing medical records, and applying E/M codes that reflect the actual services provided by health care providers in both outpatient services and hospital settings.
- **Healthcare facilities**: Hospitals, clinics, nursing homes, and other healthcare facilities rely on EM Coding to ensure accurate billing and reimbursement for the services rendered to patients. Proper coding helps healthcare facilities maintain financial stability and compliance with regulatory requirements.
- **Insurance companies**: Insurance companies use EM codes to process claims and determine the reimbursement owed to healthcare providers. They rely on these codes to assess the medical necessity of services and ensure that providers are billing appropriately for the care delivered.
- **Government agencies**: Medicaid services and Medicare use E/M coding to reimburse healthcare professionals, guide audits, and shape policy decisions that affect evaluation and management services across the nation.
- **Healthcare administrators**: Healthcare administrators use EM Coding data for financial planning, resource allocation, and performance monitoring within healthcare organizations. They rely on accurate coding to assess productivity, track patient demographics, and identify areas for improvement in healthcare delivery.
## **Reference**
American Academy of Professional Coders. (2024). What are E/M codes? https://www.aapc.com/resources/what-are-e-m-codes