Dissociation is typically measured using standardized scales such as the Dissociative Experiences Scale (DES). The DES is a self-report instrument that assesses the frequency and intensity of dissociative symptoms, including depersonalization, derealization, and amnesia. The DES is widely used in both clinical and non-clinical samples to evaluate dissociative experiences and identify potential dissociative disorders.
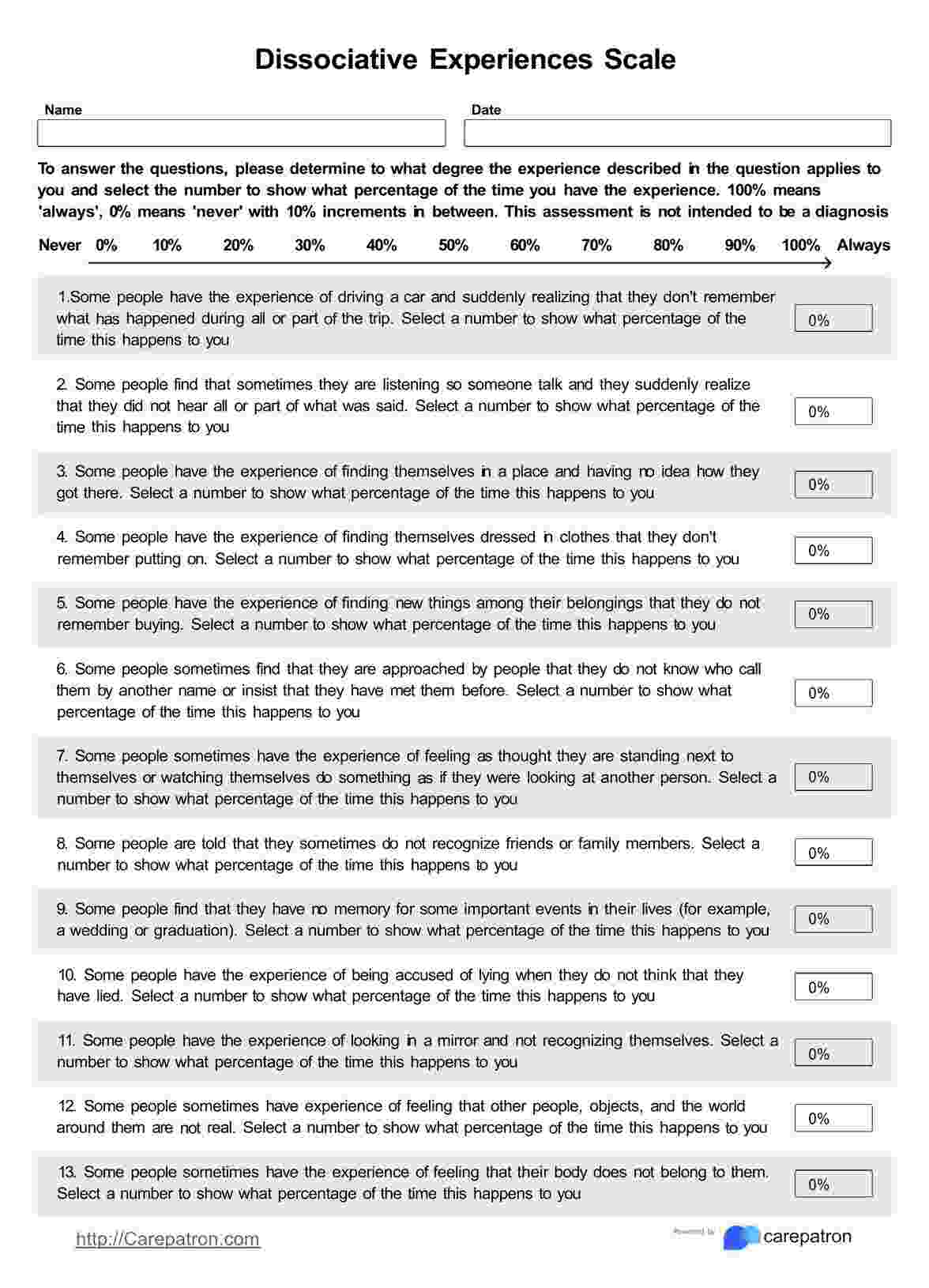
Dissociative Experiences Scale
The Dissociative Experiences Scale is a clinical screening tool that assesses dissociation in patients. Download this PDF to evaluate dissociative tendencies.
Dissociative Experiences Scale Template
Commonly asked questions
The stages of dissociation are not strictly defined but can be broadly categorized into three stages: (1) mild dissociation, characterized by brief episodes of depersonalization or derealization; (2) moderate dissociation, marked by increased frequency and duration of dissociative episodes; and (3) severe dissociation, characterized by significant impairment in daily functioning and a high frequency of dissociative episodes.
A normal score for the DES typically falls below 20, indicating minimal dissociative symptoms. Scores above 20 are generally considered indicative of dissociative disorders, such as dissociative identity disorder or depersonalization disorder. However, high scores do not necessarily mean a more severe dissociative disorder is present, as the scale measures both normal and pathological dissociation.
EHR and practice management software
Get started for free
*No credit card required
Free
$0/usd
Unlimited clients
Telehealth
1GB of storage
Client portal text
Automated billing and online payments











