Looking for a tool to help you record the specific activities of daily living your patients are capable of doing? Read our guide to learn about the activities of daily living and obtain an Activities of Daily Living to check your patient's independence, assess if they can live independently, to better inform your care plan, eligibility for long-term care, etc.
## **What are the Activities of Daily Living?**
Activities of daily living (ADLs) are essential tasks that individuals perform daily to maintain their independence and well-being. For healthcare practitioners, understanding and assessing ADLs is crucial in providing comprehensive care, especially for older adults and those with cognitive impairments. This guide explores the concept of ADLs, assessment tools, and their importance in healthcare settings.
Activities of daily living encompass a range of basic and instrumental tasks necessary for independent living. These activities are broadly categorized into two groups (Edemekong et al., 2025):
### **1. Basic activities of daily living (BADLs)**
Basic ADLs include fundamental self-care tasks or personal care tasks such as:
- Personal hygiene (bathing, grooming, nail care), including dental hygiene
- Dressing (from selecting appropriate clothes to putting them on)
- Eating
- Toileting or having control of bladder and bowel function
- Transferring (moving from bed to chair, etc.)
- Walking or functional mobility
### **2. Instrumental activities of daily living (IADLs)**
IADLs are more complex tasks that support independent living:
- Meal preparation
- Managing medications
- Managing finances and paying bills
- Housekeeping and home maintenance
- Using public transportation
- Shopping
- Using communication devices
- Doing laundry
In the 2012 National Health Interview Survey Report by the Centers for Disease Control and Prevention, around 5 million people (2%) depend on assistance from others for activities of daily living, and roughly 10 million people (4%) need help with instrumental activities of daily living.
A person's capacity to perform activities of daily living (ADLs)can be negatively affected by a wide range of factors. These primarily include a decline or impairment in physical or cognitive function. Specifically, medical conditions affecting the musculoskeletal, neurological, circulatory, or sensory systems can lead to decreased physical function, making tasks like walking, bathing, or dressing difficult (Association of Health Care Journalists, 2023).
Additionally, a decline in cognitive or mental status, such as in cases of dementia or severe cognitive fluctuations, can impair a person's ability to complete both basic ADLs and more complex instrumental activities of daily living (IADLs), which require organizational and advanced thinking skills like managing finances or preparing meals.
Beyond chronic health conditions, several other factors can influence functional independence. Acute events that impact their physical health, such as a sudden injury or a hospitalization for an acute illness, are frequently associated with a rapid decline in ADL abilities.
Other contributing elements can include the adverse side effects of medications, social isolation, and environmental factors within a patient's home that may present barriers to movement and self-care (Edemekong et al., 2025). The progressive loss of ADLs is also a common consequence of the natural aging process itself, often starting with difficulty in IADLs before affecting basic self-care tasks.
## **What is an Activities of Daily Living Checklist?**
An Activities of Daily Living Checklist is a standardized assessment tool one can use to measure an individual's functional status and their ability to perform essential self-care tasks. It is a valuable resource employed by various healthcare practitioners to assess an individual's functional capacity and independence in performing essential self-care tasks. The checklist is handy in the following scenarios:
- **Geriatric assessment**: Geriatricians and healthcare professionals specializing in elder care often use the ADL Checklist to evaluate the functional status of older adults. It aids in identifying age-related declines in daily living activities and guides the development of care plans for maintaining independence.
- **Rehabilitation settings**: An occupational therapist or other rehabilitation specialists utilize the ADL Checklist to assess the progress of individuals or hospitalized patients recovering from injuries, surgeries, or debilitating conditions. The checklist helps tailor rehabilitation plans to improve specific areas of functional impairment.
- **Home healthcare services**: Home healthcare providers use the ADL Checklist to assess the needs of clients receiving home care. The checklist guides the development of personalized care plans, ensuring that caregivers, especially family caregivers, address specific challenges in daily living.
- **Assisted living and nursing homes**: Staff in assisted living communities and nursing homes employ the ADL Checklist as part of routine resident assessments. It informs the level of care provided, helps with care planning, and serves as a baseline for monitoring changes in day-to-day functioning or functional abilities.
## **How to use our Activities of Daily Living Checklist template**
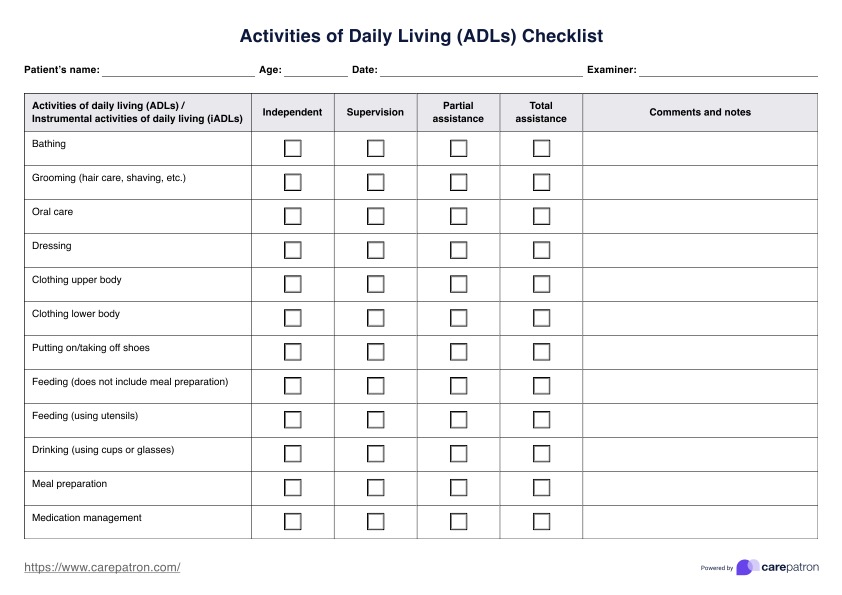
Our Activities of Daily Living Checklist template has fields for documenting both ADLs and IADLs, allowing healthcare professionals to track each patient's level of independence. The template also includes sections for notes and comments to capture additional considerations during the assessment.
### **Step 1: Access the template**
Click the "Use template" button to open the template within the Carepatron app for easy customization and sharing. If you prefer a fillable, printable format, use the “Download” button to get a PDF version.
### **Step 2: Familiarize yourself with the template**
The columns on the ADL checklist allow healthcare professionals to categorize a patient's ability to perform each task, helping to determine the level of care required. Here's an overview of what each column means:
- **Independent**: The patient can perform the activity without any help or supervision.
- **Supervision**: The patient can perform the task on their own, but may need someone to oversee or guide them for safety or support.
- **Partial assistance**: The patient can perform part of the activity but needs help to complete it.
- **Total assistance**: The patient is unable to perform the activity independently and requires full assistance.
- **Comments and notes**: This field allows for additional observations or considerations that may be relevant to the patient's performance or the overall care plan.
These columns ensure that the assessment captures the nuances of a patient's abilities and helps tailor care plans effectively.
### **Step 3: Assess the patient**
Guide the patient through each ADL and IADL task listed on the template. For each activity, note whether the patient can perform it independently, with supervision, or with partial or total assistance. Ensure the assessment reflects the patient's current abilities.
### **Step 4: Record results**
Use the columns provided to indicate the patient's level of independence for each activity. You can also add any additional notes about the patient's performance or areas that require improvement.
### **Step 5: Discuss results with the patient**
After completing the checklist, go over the results with the patient. If applicable, explain how the assessment will inform their care plan and areas that need support. This is particularly important for patients working towards regaining independence or caregivers helping in their everyday life tasks.
For a more comprehensive evaluation, healthcare professionals can combine the ADL checklist with other assessments. This multi-faceted approach can enhance diagnostic accuracy and guide long-term care planning.
## **ADL assessment tools**
Several standardized measures and functional assessment tools are available to evaluate an individual's ability to perform ADLs:
- **Katz Index of Independence in Activities of Daily Living**: The [Katz Index](https://google.com/url?sa=t&rct=j&q=&esrc=s&source=web&cd=&ved=2ahUKEwiXu9Si_6-HAxVxslYBHQfkGs0QFnoECBcQAQ&url=https%3A%2F%2Fwww.carepatron.com%2Ftemplates%2Fkatz-index-of-independence-in-activities-of-daily-living&usg=AOvVaw0c5qXFpwsDPdKsN_bcnRWM&opi=89978449) is one of the most commonly used tools to assess basic ADLs. It evaluates six functions: bathing, dressing, toileting, transferring, continence, and feeding. The index ranks the adequacy of performance in these functions and provides a simple, standardized measure of biological and psychosocial function.
-** Lawton-Brody instrumental activities of daily living scale**: This scale assesses eight domains of function related to IADLs: using the telephone, shopping, food preparation, housekeeping, laundry, transportation, medication management, and finances. It is particularly useful for identifying how a person is functioning at present and detecting improvement or deterioration over time.
- **Barthel Index**: The [Barthel Index](https://www.carepatron.com/templates/barthel-index/) measures performance in 10 activities of daily living. It is widely used to assess functional status and determine the level of assistance required for individuals with neuromuscular or musculoskeletal disorders.
- **Texas functional living scale**: This assessment tool evaluates functional abilities in individuals with mild cognitive impairment or early-stage dementia. It assesses four domains: time, money and calculation, communication, and memory.
- **Patient Specific Functional Scale**: The [PSFS](https://www.carepatron.com/templates/patient-specific-functional-scale/#app-chapter-one) is a comprehensive evaluation tool that helps medical professionals collect, organize, and store information to assess an individual's functional capabilities. Patients are asked to identify up to 5 tasks they cannot do and rate each on an 11-point scale, ranging from 0 (unable) to 10 (fully capable).
## **References**
Association of Health Care Journalists. (2023, November 9). Activities of daily living. https://healthjournalism.org/glossary-terms/activities-of-daily-living/
Centers for Disease Control and Prevention. (2013). Summary health statistics for the U.S. population: National Health Interview Survey, 2012. https://www.cdc.gov/nchs/data/series/sr_10/sr10_259.pdf
Edemekong, P. F., Bomgaars, D. L., Sukesh Sukumaran, & Schoo, C. (2025, May 4). Activities of daily living. StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK470404/