What is a Massage Therapy Soap Note?
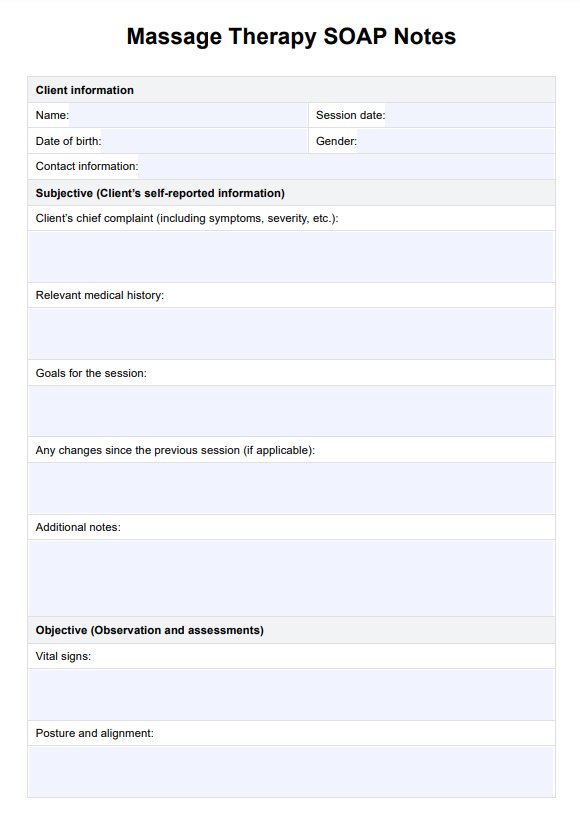
A SOAP note for massage therapy is a vital and structured documentation tool massage therapists use to effectively record and track their clients’ treatment progress. The acronym “SOAP” stands for Subjective, Objective, Assessment, and Plan, representing the note’s four critical components.
In the Subjective section, therapists document the client’s self-reported information, such as their presenting concerns, symptoms, and goals for the session. This provides valuable insights into the client’s perspective and helps the therapist tailor the treatment accordingly.
The Objective section comprises the therapist’s objective observations during the session. This includes the therapist’s assessment of the client’s physical condition, range of motion, muscle tension, and noteworthy findings. Objective data is crucial for tracking changes over time and evaluating the effectiveness of the treatment.
The Assessment component involves the therapist’s professional analysis of the client’s condition based on both subjective and objective information. It helps identify patterns, progress, and potential areas needing further attention.
The Plan section outlines the therapist’s proposed plan for future sessions. This may involve specific techniques, focus areas, and self-care recommendations between sessions. It ensures continuity of care and enables the massage therapist to collaborate effectively with the client.
Massage Therapy SOAP Notes offer several benefits. They enhance communication between therapists and clients, ensuring that treatment goals are aligned and progress is tracked. These SOAP notes also facilitate collaboration among healthcare professionals if the client receives care from multiple sources.
Moreover, effective SOAP Notes assist in maintaining accurate and organized records, which is essential for legal and ethical reasons. They provide a comprehensive history of the client’s sessions, which can be helpful in case of insurance claims, audits, or legal disputes.
In general, Therapy SOAP Notes serve as a comprehensive record-keeping system that helps therapists provide high-quality, individualized care to their clients. By capturing relevant information and facilitating informed decision-making, SOAP Notes contribute to the overall success of massage therapy treatments and promote clients’ well-being.