The IgE antibody
The IgE antibody, or Immunoglobulin E, is a class of antibodies primarily associated with allergic reactions and asthma. It plays a crucial role in the body's immune response to allergens. When an allergen enters the body, it triggers the production of specific IgE antibodies. These antibodies bind to immune cells like mast cells and basophils, releasing inflammatory substances like histamine, which cause the symptoms of an allergic reaction.
IgE is also involved in immunity against parasites. However, in developing countries with less common parasitic infections, IgE is more associated with allergies and allergic diseases such as hay fever, food allergies, and atopic dermatitis.
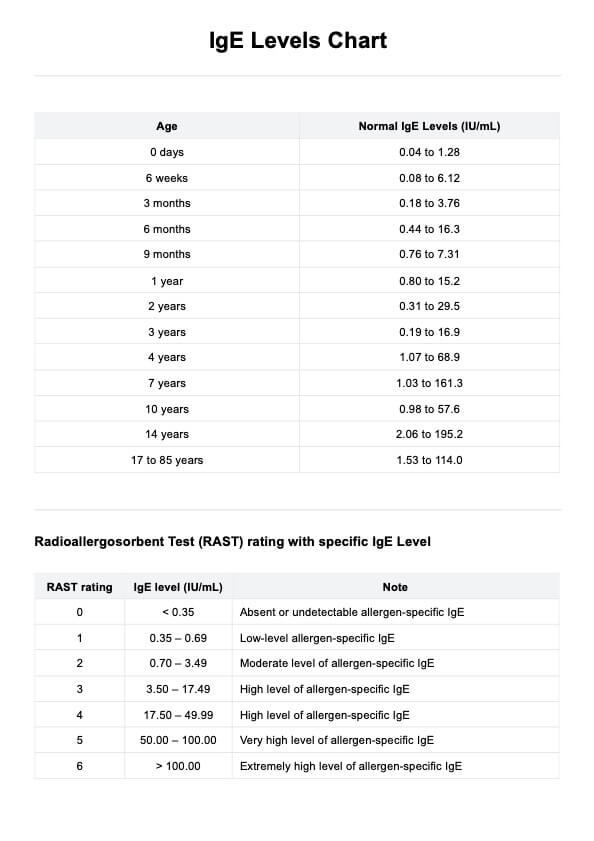
Understanding IgE levels can be important for diagnosing and managing allergic diseases. Elevated IgE levels can indicate allergic sensitivity, but they must be interpreted in the context of clinical history and specific allergen testing. The Radioallergosorbent Test (RAST) is one method used to measure specific IgE antibodies to particular allergens, helping to pinpoint specific allergic triggers.