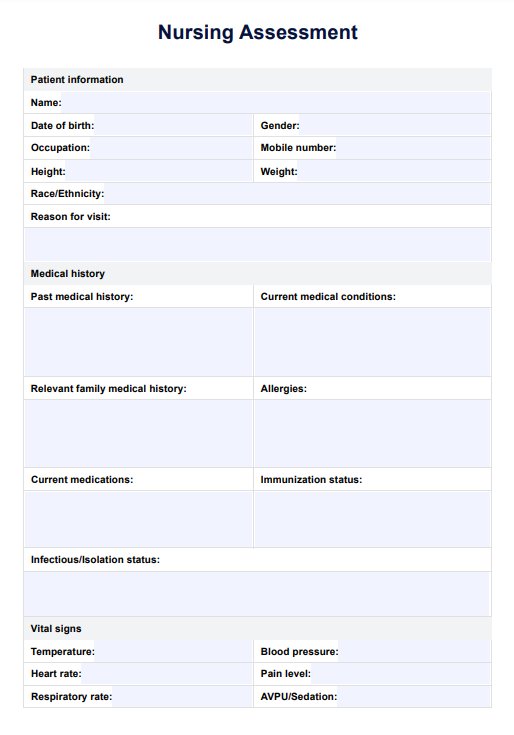
What is a Nursing Assessment?
A Nursing Assessment involves collecting comprehensive information about a patient's physical, psychological, and social health to develop a personalized care plan. This assessment is crucial for ensuring patient safety and guiding the healthcare team.
During a head-to-toe assessment, nurses gather both subjective and objective data. Subjective data refers to what the patient shares, such as symptoms or pain levels. Objective data comes from measurable findings during a physical assessment, such as vital signs, including blood pressure, pulse, and respiratory assessment. Nurses may also listen for bowel sounds and assess the patient's overall condition.
Nursing Assessments happen during various stages, such as admission assessments, routine check-ups, or when there's a change in the patient's status. These assessments may be comprehensive or focused assessments targeting specific areas of concern. During this nursing process, nurses use the gathered data to make informed clinical judgments and create a nursing diagnosis.
By conducting thorough assessments, nurses help identify health issues early, prevent complications, and ensure the patient receives the best possible care. These assessments also improve communication between nurses and other health professionals, contributing to effective collaboration within the health care team.