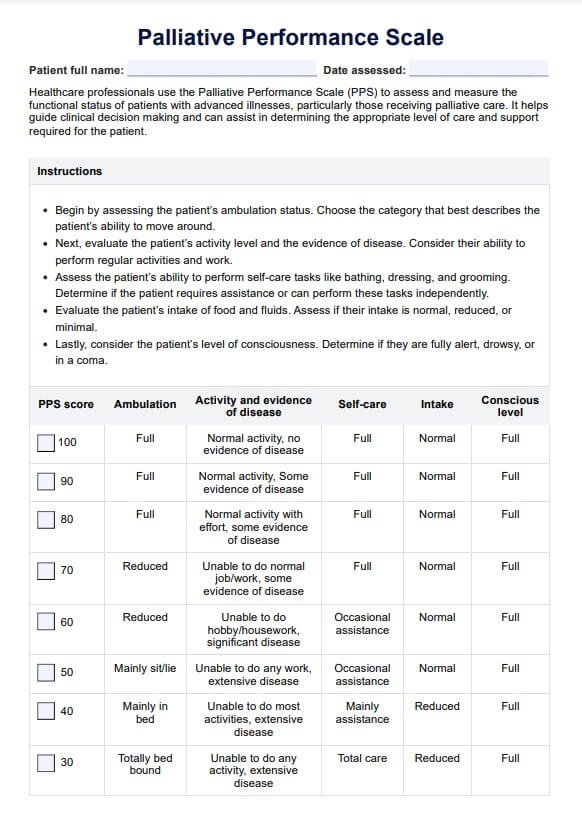
What is a Palliative Performance Scale (PPS)?
The Palliative Performance Scale (PPS) is a reliable and valid tool based on and derived from the Karnofsky Performance Scale (KPS). Healthcare professionals use it to assess the functional status of palliative care patients, commonly advanced cancer patients or those with a significant disease like chronic obstructive pulmonary disease (Anderson et al., 1996).
The PPS comprehensively evaluates a patient's ability to perform daily activities and addresses physical decline, level of consciousness, and the need for assistance. This is an 11-point scale ranging from 0% to 100%, with 10% increments. Each score represents a specific level of functional ability and describes the extent of assistance required for self-care activities, such as ambulation, activity level, evidence of disease, intake, and consciousness level (Ho et al., 2008). This makes it an essential tool to those who provide a palliative medicine consultation service because it can help determine disease trajectory, and a clear disease trajectory predicts survival estimates.
At the higher end of the scale, a score of 100% indicates a fully ambulatory patient with normal activity levels and self-care abilities with minimal or no help. As the score decreases, the patient's functional status declines, indicating a greater need for assistance and a higher level of palliative care interventions.
The PPS scale is widely used in palliative care settings, including hospice care and a palliative care unit, to assess a patient's eligibility for services and to guide care planning. Patients with a PPS score of 70% or lower are generally considered appropriate candidates for hospice care, as they typically require considerable assistance with self-care activities and have limited life expectancy.