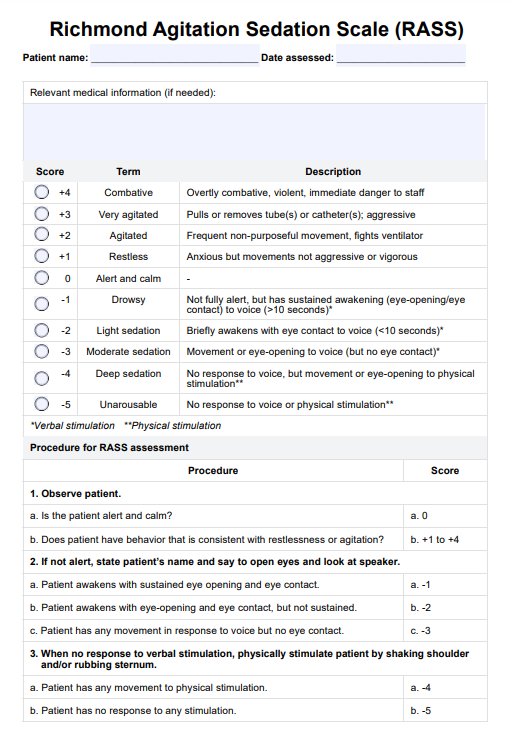
How to use the Richmond Agitation Sedation Scale (RASS)?
After obtaining a copy of the Richmond Agitation Sedation Scale PDF template, follow the steps to make the most out of the template:
Step 1: Observe patient
Observe the patient while undergoing treatment in an emergency room or intensive care unit. To properly assign specific scores to the patient, the professional using the RASS Scale needs to observe the patient answer the following questions:
- While they are being treated, is the patient alert? Are they calm? Are they exhibiting any signs of being restless or agitated? Depending on what you notice, this may score anywhere between 0 to +4
- If they are not alert, they are likely in light sedation. If that's the case, try saying your patient's name in a loud speaking voice. Prompt patient and direct patient to open their eyes and look at you. If they are still unresponsive the first time around, you may choose to repeat this once or twice. If they do respond, you may also tell them to continue looking at you as you talk to them. Depending on what you notice, this may score anywhere between -1 and -3.
- If they don't respond to your voice at all, they are likely to be deeply sedated. Physically stimulate patient by shaking their shoulder. If they don't respond to that, rub their sternum. They will either get a score of -4 or -5, signifying a deep sedation protocol, depending on if they respond to being physically nudged or if they don't respond at all.
Step 2: Assign a RASS score
As discussed above, the RASS Scale is scored between -5 and +4. The negative values measure sedation, while the positive values rate agitation. This scale is relatively easy to use because it has a set scoring system with specific designations.
What healthcare professionals need to aim for when using this scale is to get to the point where the patient will score between -2 and +1, which means they are properly sedated. However, this will depend on the sedation protocols for the kind of illness or injury they are treating. It is important to use sedative medications in conjunction with the RASS for effective patient management.