What is a Spinal Nerve Diagram?
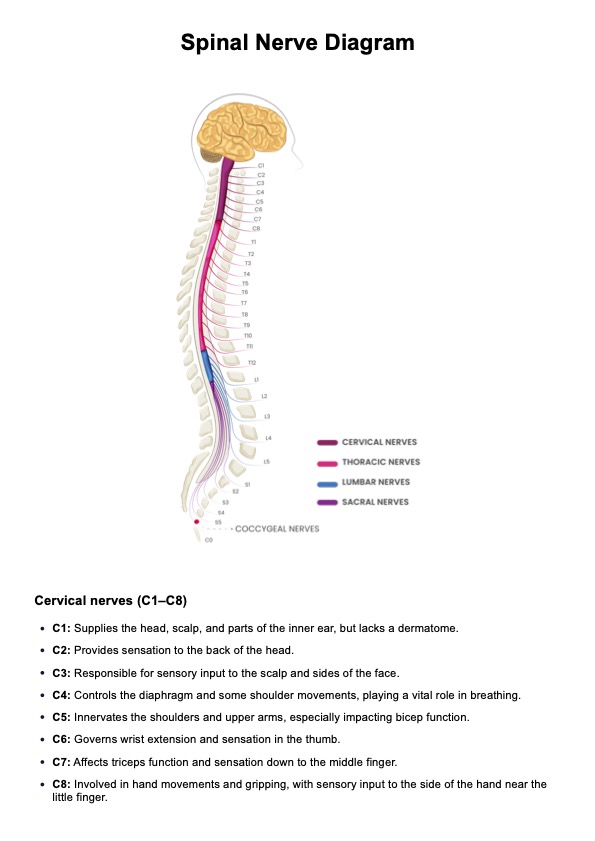
A Spinal Nerve Diagram is a vital resource for healthcare professionals, offering a detailed illustration of the spinal nerves and their respective functions. This chart visually represents the 31 pairs of spinal nerves that branch out from the spinal cord. These nerves are critical for transmitting sensory and motor signals between the brain, spinal cord, and various parts of the body, allowing for coordinated movement and sensation.
Each spinal nerve is connected to a specific region of the body, forming an essential part of both the central nervous system and the peripheral nervous system (Thau et al., 2022). The spinal nerves originate from the spinal cord, with their spinal nerve roots emerging from different sections of the spine. These nerve roots then branch into various peripheral nerves that control sensation and motor function in corresponding areas (Harrow-Mortelliti, 2023; Kaiser, 2019):
- Cervical spinal nerves (C1-C8): The cervical nerves emerge from the cervical portion of the spine and innervate the neck, shoulders, arms, and hands. Dysfunction in the cervical spinal nerves can lead to issues such as weakness or numbness in the upper extremities, as seen in conditions like cervical radiculopathy.
- Thoracic spinal nerves (T1-T12): The thoracic spinal nerves control the muscles in the chest, upper back, and parts of the abdomen. They help stabilize the trunk and assist with respiration. Damage to these nerves may cause issues like thoracic radiculopathy, which can result in chest pain or abdominal discomfort, mimicking other conditions.
- Lumbar spinal nerves (L1-L5): The lumbar spine nerves extend from the lumbar region of the spine and play a critical role in controlling the lower back, hips, and legs. Conditions affecting the lumbar spinal nerves, such as herniated discs or lumbar radiculopathy, may cause lower back pain, sciatica, or weakness in the legs.
- Sacral spinal nerves (S1-S5): Emerging from the sacral region, the sacral spinal nerves influence the pelvic area, thighs, legs, and feet. Disorders of these nerves can lead to issues such as sacral radiculopathy, which often presents as sciatica, causing pain to radiate down the legs.
- Coccygeal nerves (Co): These nerves arise from the coccyx, or tailbone, and have a more limited role in sensation and movement, primarily affecting the area around the coccyx. Issues with the coccygeal nerves are less common but can cause pain in the lower spine or tailbone region, known as coccydynia.
Knowing how these nerves relate to specific body parts is essential in diagnosing conditions such as herniated discs, spinal stenosis, sciatica, and radiculopathy. Using this diagram, healthcare professionals can better pinpoint nerve damage and manage their patients' associated symptoms.