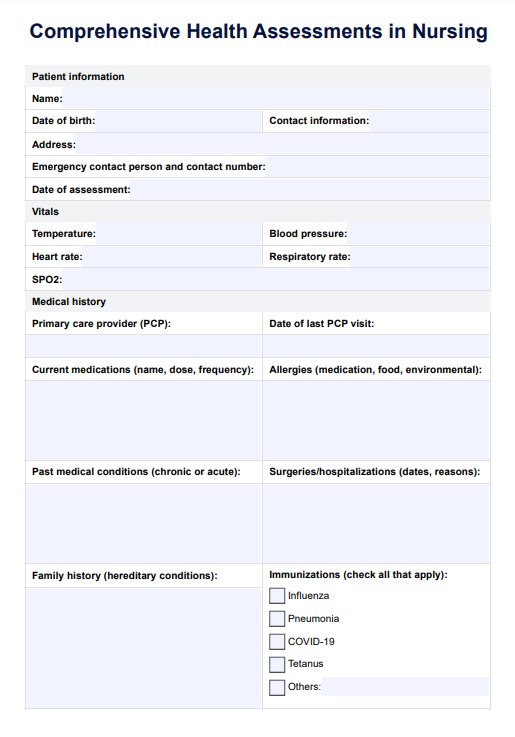
What is a comprehensive health assessment in Nursing?
A Comprehensive Health Assessment in Nursing systematically and thoroughly examines an individual's physical, mental, and emotional well-being. It is a foundational element in healthcare (specifically nursing practice), providing a holistic view of a patient's health status and aiding a healthcare team in forming sound clinical judgment.
This type of health assessment goes beyond the immediate health concerns and delves into various aspects of a person's life, contributing valuable information for personalized care plans.
The critical components of a comprehensive health assessment are:
- Psychosocial assessment: It is crucial to understand the patients admitted and their mental and emotional state. This focused assessment evaluates their mental health, social support systems, lifestyle factors, and any psychosocial stressors that may impact their well-being.
- Medical history: It is essential to gather a comprehensive medical history. This includes information about past health history, illnesses, surgeries, medication history, allergies, and family medical history.
- Cultural considerations: Recognizing the influence of cultural factors is crucial in providing patient-centered care. A comprehensive health assessment considers the patient's cultural background, beliefs, and practices.
- Head-to-toe assessment: Nurses conduct a detailed Head-to-Toe Assessment assessing vital signs, specific body systems, and overall body function. This helps identify any existing health status and potential risks. This physical examination helps in obtaining objective data.