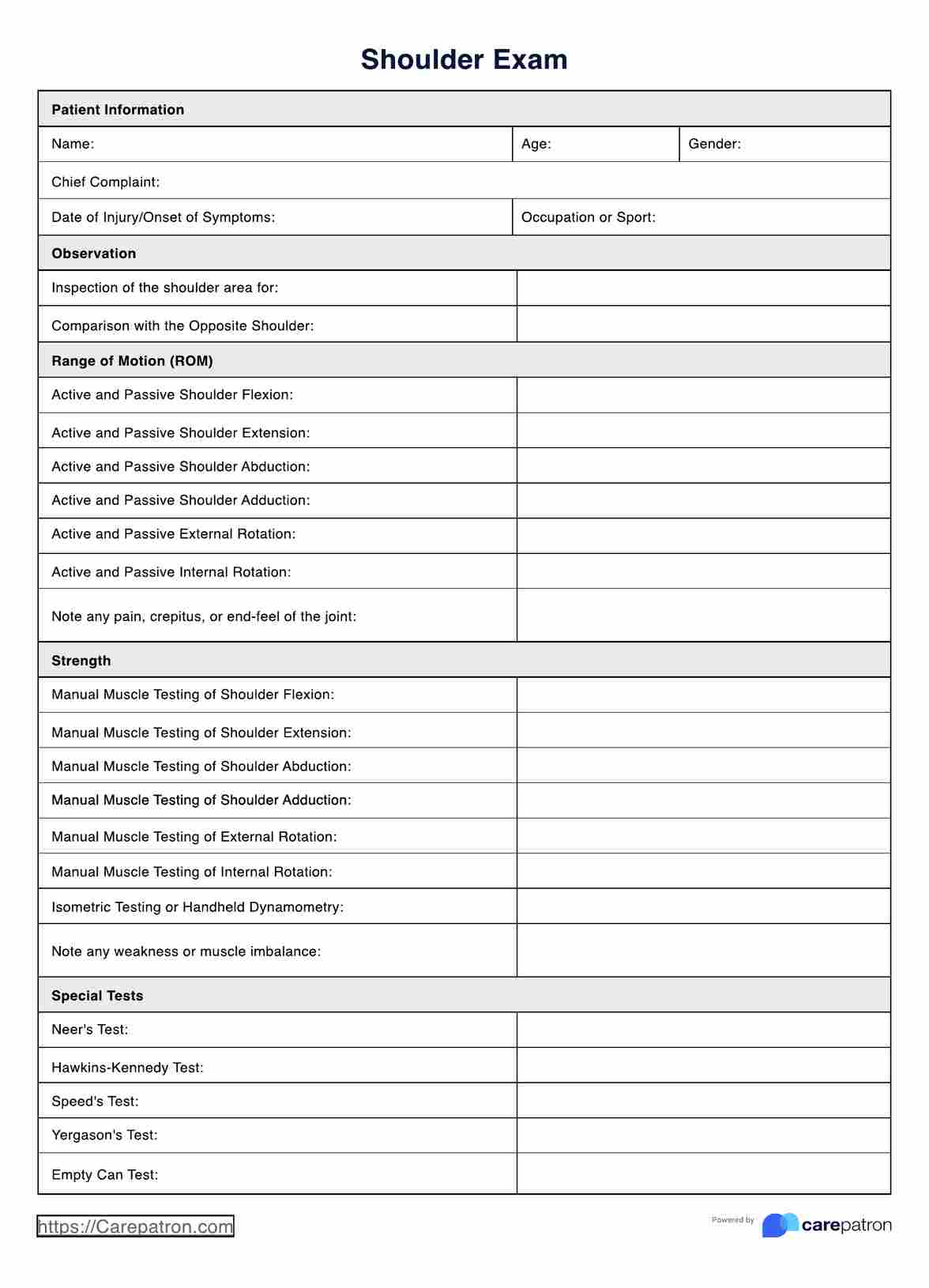
How to use this Shoulder Exam
Physical therapists employ the Shoulder Exam to address shoulder dysfunction, anterior shoulder pain, shoulder dislocation, impingement, rotator cuff tear and tendonitis, and other related pathologies.
Step 1: Collect patient information
Initiate the process by compiling the patient's essential personal and medical details, including their name, age, gender, chief complaint, date of injury or symptom onset, and occupation or sports involvement.
Step 2: Conduct observations
For initial assessment, position the patient standing. Thoroughly inspect the shoulder area for indications of swelling, deformities, redness, or muscle atrophy. Compare the injured shoulder with its counterpart to discern alignment, posture, or overall appearance disparities.
Step 3: Evaluate range of motion (ROM)
Systematically appraise the shoulder joint's active and passive ROM, encompassing flexion, extension, abduction, adduction, internal rotation, external rotation, and forward flexion. Take note of any pain, crepitus, or irregular end-feel during joint movement.
Step 4: Assess strength
Evaluate muscle strength in the shoulder joint through manual muscle testing, isometric testing, or handheld dynamometry. Identify weaknesses, muscle imbalances, or compensatory movements that may manifest during strength testing.
Step 5: Perform special tests
Execute specialized tests such as Neer's Test, Hawkins-Kennedy Test, Speed's Test, Yergason's Test, Empty Can Test, Drop Arm Test, Apprehension Test, and Relocation Test to pinpoint specific shoulder pathologies or impingements. These tests are beneficial for evaluating the biceps tendon, including conditions like biceps tendonitis and instability.
Step 6: Palpate the shoulder area
Utilize palpation to examine the shoulder joint, clavicle, scapula, acromioclavicular joint, coracoid process, bicipital groove, and surrounding soft tissues for signs of tenderness, swelling, or deformities.
Step 7: Evaluate functional deficits
Identify functional deficits by assessing limitations or challenges in daily activities such as overhead reaching, dressing, and lifting. Additionally, scrutinize for deficits in sports-specific movements or occupational tasks. Assessing the patient's arm during these functional activities is crucial to identify specific limitations and guide appropriate interventions.
Step 8: Order additional tests if needed
If necessary, prescribe additional imaging studies such as X-rays, MRI, or ultrasound to confirm or rule out specific diagnoses.
Step 9: Develop a tailored treatment plan
Based on the findings from the Shoulder Exam, construct a personalized treatment plan encompassing targeted exercises, manual therapy techniques, activity modifications, and patient education to address the diagnosed shoulder pathology and associated functional deficits. Regularly reassess the patient's progress and adjust the treatment plan as warranted.