What is oral allergy syndrome?
Oral allergy syndrome (OAS), also known as pollen food allergy syndrome, is an allergic condition that occurs when certain proteins in raw fruits, vegetables, or nuts cross-react with pollen allergens (American Academy of Allergy Asthma & Immunology, 2021). It commonly affects individuals with hay fever or seasonal allergies, particularly during peak pollen season. OAS symptoms are typically mild and localized to the mouth and throat, including itching, tingling, or swelling after consuming the triggering foods.
This reaction is not a traditional food allergy but is closely linked to pollen allergies, such as birch tree, weed, or grass pollen. For example, people allergic to birch pollen may react to apples, carrots, or almonds. While symptoms are usually mild, some cases can escalate into a severe allergic reaction, though this is rare.
To diagnose oral allergy syndrome, healthcare practitioners assess the patient's history, seasonal allergy patterns, and specific food triggers. Skin tests or blood tests may confirm sensitivities to pollen or related allergens. While oral allergy syndrome is typically treated by avoiding triggering foods, cooking can neutralize the proteins and prevent reactions. Practitioners should educate patients about managing mild symptoms and recognizing signs of severe allergic reactions to ensure safety and improve quality of life.
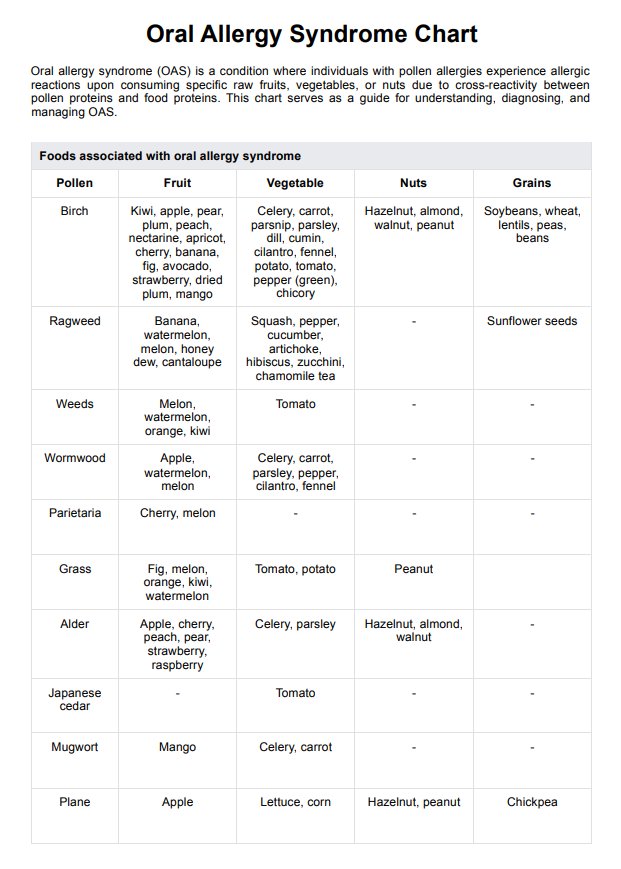
Foods associated with oral allergy syndrome
Oral allergy syndrome is triggered by proteins in various foods that cross-react with pollen allergens (Kashyap & Kashyap, 2015). Common food categories include fruits, vegetables, nuts, grains, and seeds. Specific triggers often align with the type of pollen allergy a person has.
Birch pollen is linked to reactions from apples, kiwis, pears, peaches, celery, carrots, hazelnuts, and almonds. Ragweed-related OAS symptoms may occur with bananas, melons, squashes, and zucchini (Pastorello et al., 2000). Grass pollen is associated with figs, melons, oranges, potatoes, and peanuts, while mugwort can trigger reactions from mangos, celery, and carrots. Additionally, alder pollen may cause sensitivities to cherries, peaches, and hazelnuts.
Cooking or processing these foods can often neutralize the proteins, reducing the risk of an allergic reaction. Healthcare professionals should guide patients in identifying triggers and managing their diets during pollen-heavy seasons to minimize OAS symptoms and maintain nutritional balance.