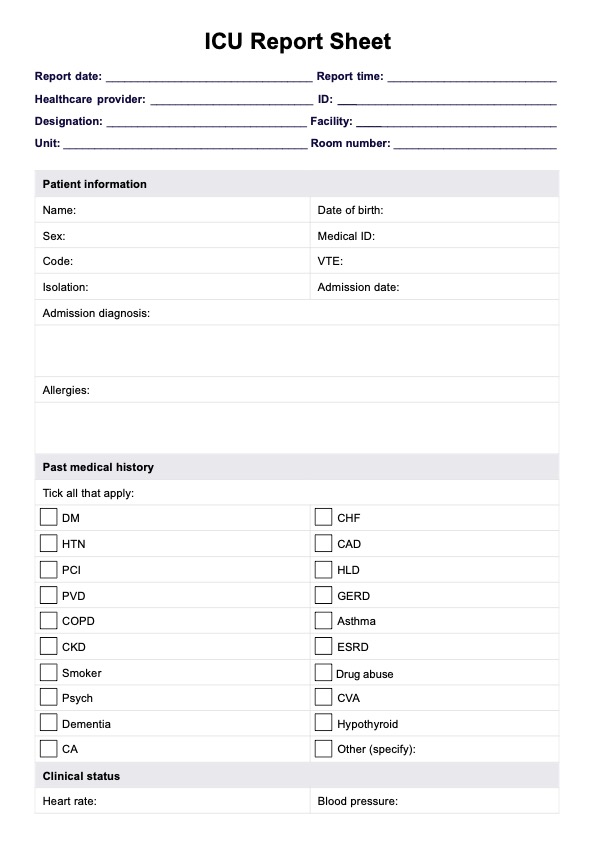
What is an ICU Report Sheet Template?
An ICU (Intensive Care Unit) Report Sheet Template is a structured document used by healthcare professionals (particularly ICU nurses and other critical care team members). These documents organize and communicate important information during shift handovers or daily rounds in an intensive care setting.
The purpose of ICU report sheets is to streamline communication and ensure that crucial patient details are accurately and efficiently transferred between healthcare providers, promoting continuity of care and patient safety. These documents help ICU nurses stay organized, facilitate consistent communication, and ensure coordinated healthcare.
Common elements in an ICU nursing report include:
- Patient information: Basic demographics, such as name, age, and medical record number.
- Admission diagnosis: The primary reason the patient was admitted to the ICU.
- Medical history: Relevant past medical history that may impact the current care.
- Current diagnosis and clinical status: A summary of the patient's current condition, including vital signs, neurological status, and any ongoing interventions.
- Ventilator settings and parameters: Details about mechanical vent settings, if applicable, including settings and any changes made.
- Medications: A list of drugs administered, including doses and times.
- Laboratory results: Critical values and pertinent laboratory findings.
- Procedures and interventions: Documentation of any procedures performed or interventions initiated.
- Special considerations: Any unique considerations or specific care needs for the patient.
- Upcoming events or plans: Anticipate the forthcoming procedures, tests, or changes in the care plan.
A filled-out report acts as a quick reference tool, allowing you and your team to grasp a patient's overall status efficiently. It promotes a standardized approach to information transfer, reducing the risk of errors and oversights during shift changes. By using a template, healthcare professionals can ensure that essential details are consistently documented in a way that everyone understands.