What is the Insomnia Severity Index (ISI)?
The Insomnia Severity Index (ISI) is a 7-item self-report questionnaire that evaluates insomnia’s nature, severity, and impact over the past month. It assesses several dimensions of sleep disturbances, including difficulty falling asleep, staying asleep (wake after sleep onset), and waking up too early. The ISI is also used to evaluate sleep disorders.
The ISI also measures sleep dissatisfaction, the interference of sleep problems with daytime functioning, the noticeability of sleep issues by others, and the distress caused by these sleep difficulties.
Psychometric studies have demonstrated the ISI’s ability to detect insomnia cases and evaluate treatment responses. In a community population-based sample, a cutoff score of 10 had 86.1% sensitivity and 87.7% specificity for identifying insomnia. The ISI also shows good internal consistency (Cronbach’s α = 0.90-0.91) and correlates well with sleep diaries, polysomnography, and clinical interviews (Morin et al., 2011).
The ISI has been validated in various populations, including English, Spanish, French, Arabic, Hindi, German, Korean, Chinese, and other languages. It is available in patient, clinician, and significant other versions, though the patient self-report form is most commonly used. The ISI is a widely used instrument for screening and monitoring treatment outcomes in insomnia research and clinical practice.
How is the index scored and how are the results interpreted?
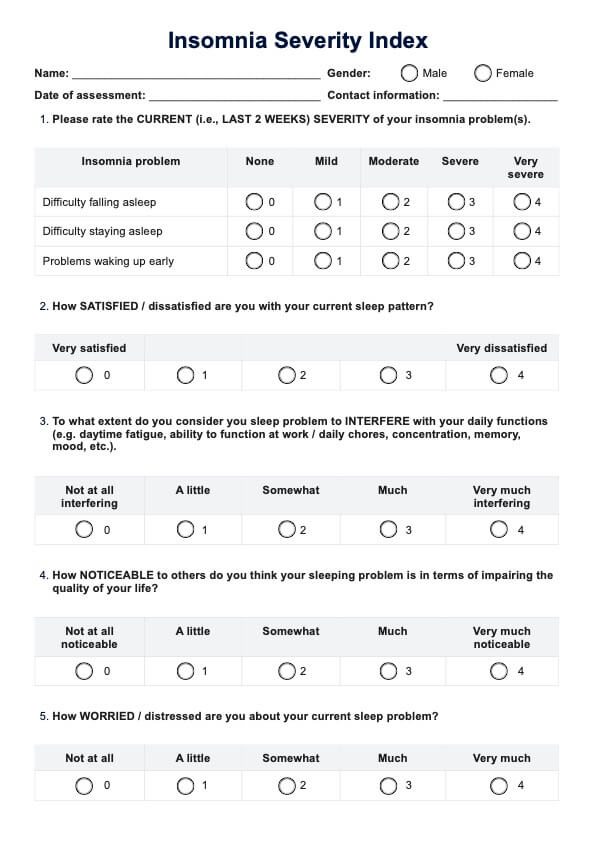
Using a 5-point Likert scale (0 = no problem to 4 = very severe problem), each of the seven items yields a total score ranging from 0 to 28. Here's how to interpret the total scores in this assessment of insomnia:
- 0–7: No clinically significant insomnia
- 8–14: Subthreshold insomnia
- 15–21: Moderate insomnia
- 22–28: Severe insomnia
Next steps after using this index
After administering the ISI, interpret scores to detect cases of insomnia and determine severity using the original ISI cutoff scores. Additional moderate to severe insomnia assessments, such as a self-report questionnaire assessing sleep onset latency and the Pittsburgh Sleep Quality Index, should be considered. Evaluating poor sleep quality using additional tools can provide valuable insights into sleep disturbances.
Discuss results with the patient to develop a treatment plan, which may include therapy, medication for persistent insomnia, and addressing sleep maintenance and early morning awakenings. Track progress using valid instruments and aim for an 8.4-point (95 CI) improvement in ISI scores, indicating reduced insomnia symptoms.
Consider a possible history of insomnia and be vigilant for comorbid conditions like sleep apnea. Early detection and intervention are crucial, as insomnia often remains unrecognized and untreated.