Patient assessment
Evaluate the patient's response to stimuli
During this assessment, clinicians carefully observe how the patient reacts to verbal and tactile stimuli. A quick and appropriate response is indicative of a higher level of consciousness. Whether responding to a spoken question or a gentle touch, the patient's ability to engage with stimuli provides valuable insights into the integrity of their neurological functions.
Observe for signs of confusion, lethargy, or agitation
Behavioral cues play a crucial role in gauging a patient's mental state and can serve as indicators of changes in consciousness. Observing signs of confusion, lethargy, or agitation provides clinicians with qualitative information about the patient's cognitive functioning. Changes in behavior may suggest alterations in neurological or altered mental status itself, prompting further investigation and intervention.
Evaluate orientation
To assess orientation, clinicians determine the patient's awareness of their surroundings, including person, place, time, and situation. An oriented patient demonstrates intact and normal cognitive functioning, accurately recognizing themselves, their location, the current time, and an understanding of the situation. This evaluation is essential for establishing a baseline cognitive state and monitoring deviations over time.
Identify any disorientation or memory deficits
Clinicians must be attentive and alert to any disorientation or memory deficits during patient assessment. Disorientation, where patients may appear confused about their surroundings or exhibit memory lapses, could indicate underlying neurological issues. Identifying such deficits helps guide further diagnostic evaluation and appropriate interventions.
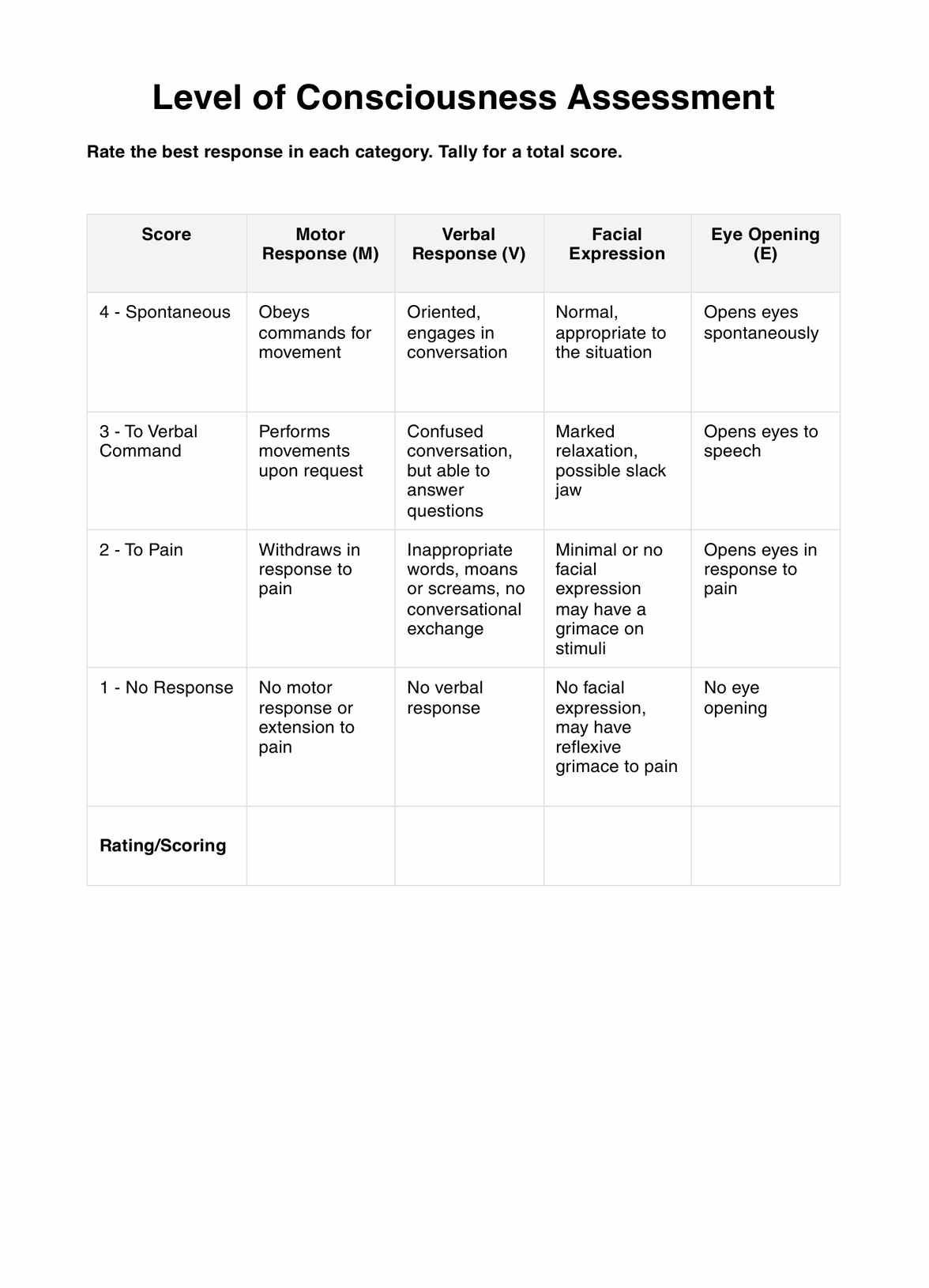
Utilize Glasgow Coma Scale (GCS)
The Glasgow Coma Scale serves as a standardized tool for quantifying the level of consciousness based on eye, verbal, and motor responses. By applying the GCS, clinicians assign a numerical score that aids in categorizing the severity of impairment. This systematic evaluation assists in objectively assessing a patient's neurological status, facilitating communication among healthcare providers, and guiding treatment decisions.
Apply the GCS
Breaking down the GCS, clinicians assess the patient's eye response, evaluating their ability to open their eyes spontaneously or respond to stimuli. The patient's verbal response is then analyzed, considering the appropriateness and coherence of the patient's verbal interactions. Finally, the motor response is observed, including the patient's ability to follow commands or exhibit purposeful movements. This comprehensive evaluation using the GCS provides a structured and quantitative approach to understanding the patient's level of consciousness.