What is hypoglycemia?
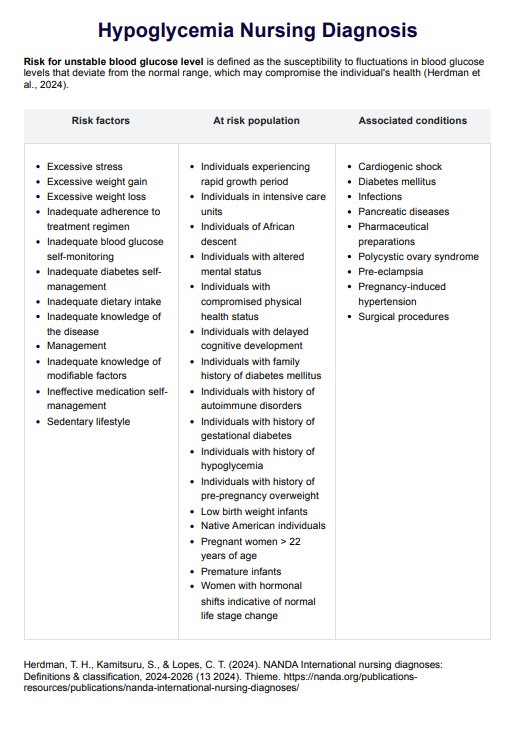
Hypoglycemia is a condition characterized by unstable blood glucose levels, specifically low blood glucose levels below the normal range, often leading to symptoms like confusion, dizziness, and sweating.
In nursing practice, a nursing diagnosis for hypoglycemia focuses on identifying risk factors such as poor nutrition, insulin overuse, or medication mismanagement. Monitoring blood glucose levels is essential to detect unstable blood glucose and intervene promptly. The goal is to maintain blood glucose levels within a safe range to prevent further complications. Nurses must assess and document unstable blood glucose trends while educating patients on managing their condition to avoid future episodes.
Symptoms of hypoglycemia
When blood glucose levels drop significantly, it can lead to symptoms requiring immediate attention. These symptoms reflect the body's response to low blood sugar and its impact on glucose metabolism. Here's a list of key symptoms:
- Sweating
- Shakiness or tremors
- Dizziness
- Rapid heartbeat
- Confusion or irritability
- Weakness or fatigue
- Blurred vision
- Hunger
In severe cases, plasma glucose concentrations can fall below 70 mg/dL, leading to seizures or unconsciousness. Early detection through frequent glucose monitoring is critical for patients on insulin or oral hypoglycemic agents to prevent hypoglycemia from occurring.
Causes of hypoglycemia
Hypoglycemia occurs when blood glucose levels fall below the normal range. Understanding the causes helps in better management and patient education to maintain stable blood glucose levels. Key causes include:
- Excessive insulin administration
- Skipping meals or delayed eating
- Alcohol consumption, especially on an empty stomach
- Excessive physical activity without adjusting food intake
- Certain medications, like oral hypoglycemic agents
- Poor blood glucose control
These factors can disturb normal blood glucose regulation, leading to symptoms of hypoglycemia. Proper monitoring of blood glucose levels and individualized care plans are essential to prevent hypoglycemia in at-risk patients.