A chiropractor note aims to record the essential information covered during the session. This includes the patient's injury, symptoms, interventions, responses, tests, assessments, and your interpretation of these factors. The specific information that you include in the chiropractor's note will depend on the session you have with your patient, but you should aim to record all pieces of vital information in your note. Having this information documented will allow you to make more informed clinical decisions, assisting the progression of the patient's treatment.
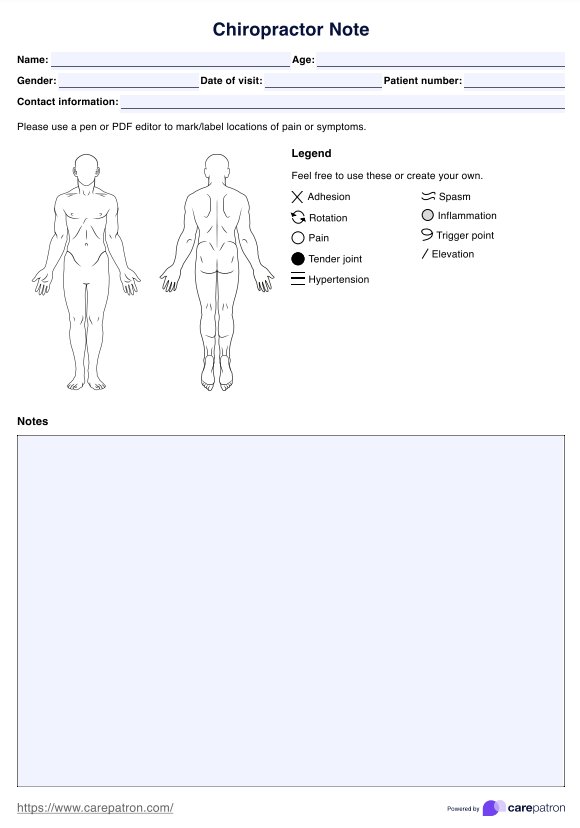
Chiropractor Note Template
Access and utilize an intuitive chiropractor note template designed to simplify documentation while improving the accuracy and organization of your notes.
Chiropractor Note Template Template
Commonly asked questions
The template improves practice efficiency by offering a standardized format for tracking patient's symptoms, neck pain, and treatment progress. It also ensures that all relevant information is captured, which is crucial for developing accurate treatment plans and monitoring future treatment outcomes.
Using a chiropractor note template helps practitioners adjust treatment plans based on objective findings and enhances the patient's well-being. By regularly updating the template, chiropractors can better monitor patient's progress and make informed decisions about ongoing care.
EHR and practice management software
Get started for free
*No credit card required
Free
$0/usd
Unlimited clients
Telehealth
1GB of storage
Client portal text
Automated billing and online payments











